The Delta Dispatch
Why First Responders Use Vital Signs: A comprehensive guide
Vital signs are measurements of the body's basic functions and are used to assess a person's overall health and wellbeing. There are four primary vital signs: body temperature, pulse rate, blood pressure, and respiratory rate. Each vital sign provides important information about a person's health and can help identify underlying health conditions or other problems.
Body temperature is a measure of the body's internal heat and is typically measured using a thermometer. A fever is generally defined as a body temperature above 100.4°F (38°C) and can indicate an infection or other underlying health condition.
Pulse rate is a measure of the heart rate, or the number of times the heart beats per minute. A rapid pulse may indicate a fever, dehydration, or an irregular heartbeat, while a slow pulse may indicate heart disease or other health conditions.
Blood pressure is a measure of the force of blood against the walls of arteries as the heart pumps blood through the body. High blood pressure, or hypertension, can increase the risk of heart disease, stroke, and other health problems.
Respiratory rate is a measure of the number of breaths a person takes per minute. A rapid respiratory rate may indicate an underlying health condition, such as asthma or pneumonia.
Monitoring vital signs is an essential part of healthcare and can help healthcare professionals and first responders make informed decisions about treatment and care.
Vital signs are measurements of basic bodily functions that are essential for assessing a person's overall health and well-being. These measurements are typically taken by healthcare professionals, but they can also be taken by trained first responders in emergency situations.
first responders attending to a patient lying on a cot outside an ambulance. One responder is checking the patient's vital signs while the other is preparing medical equipment. The patient appears to be receiving urgent medical attention, and the responders are focused and prepared to administer necessary treatment
What Are Vital Signs?
Vital signs are a set of measurements that healthcare professionals use to assess a patient's overall health status. These measurements include temperature, heart rate, blood pressure, respiratory rate, Glasgow Coma Scale (GCS), oxygen saturation (SPO2), pupils and skin.
Body Temperature:
Body temperature is an important vital sign as it can indicate whether a person is healthy or if they have a fever, which could be a sign of infection. Body temperature can be measured in several ways, including orally, rectally, or using a forehead thermometer. It is important to use the correct method and follow the manufacturer's instructions when taking a person's temperature.
Heart Rate:
Heart rate: Heart rate is the number of times the heart beats per minute and is a reflection of the heart's ability to circulate blood throughout the body. The heart rate can vary depending on age, gender, physical activity, and overall health status. A high heart rate could indicate a potential problem, such as an irregular heartbeat, dehydration, or anxiety, while a low heart rate could be a sign of a heart condition or medication side effect.
Blood Pressure:
Blood pressure is the measure of the force of blood against the walls of the arteries. It is measured in millimetres of mercury (mmHg) and consists of two numbers: the systolic pressure (the higher number) and the diastolic pressure (the lower number). A healthy blood pressure reading is typically around 120/80 mmHg. High blood pressure (hypertension) can put a strain on the heart and blood vessels, while low blood pressure (hypotension) can cause dizziness, fainting, or other symptoms.
Respiratory Rate:
Respiratory rate is the number of breaths taken per minute and is a reflection of the body's ability to take in oxygen and expel carbon dioxide. The respiratory rate can vary depending on age, physical activity, and overall health status. A high respiratory rate could indicate a potential problem, such as a lung infection or asthma, while a low respiratory rate could be a sign of respiratory depression or a medical condition that affects breathing.
Glasgow Coma Scale:
Glasgow Coma Scale or GCS measures a patient's response to verbal, motor, and eye-opening stimuli. The score ranges from 3 to 15, with a higher score indicating a higher level of consciousness. The GCS is commonly used in trauma settings to assess patients with brain injury, altered mental status, or who are sedated.
SPO2:
SPO2 is a measure of the amount of oxygen that is carried by the hemoglobin in the red blood cells. The measurement of SPO2 is non-invasive and can be performed using a pulse oximeter, which is a small device that is attached to the finger, toe, or earlobe. The pulse oximeter uses light to measure the amount of oxygen that is present in the blood.
Pupils:
Pupils can also be an important vital sign in assessing a person's neurological function. The size, shape, and reactivity of the pupils can provide valuable information about the health of the brain and nervous system. Unequal pupil size (ani or a lack of reactivity to light can be a sign of a neurological issue, such as a brain injury or nerve damage.
Skin:
Assessing skin color and moisture is important because changes in these vital signs can be indicative of underlying medical conditions. For example, changes in skin color can be a sign of poor blood flow, infection, or inflammation, while changes in skin moisture can be a sign of dehydration or certain medical conditions.
Normal Vital Sign Ranges
The normal ranges for vital signs vary depending on a person's age, gender, and health status. Here are the standard ranges:
Body Temperature:
A normal body temperature generally ranges from 36.1°C to 37.2°C, with an average of 37°C. A fever, which is typically defined as a body temperature above 38°C, can be a sign of an infection or illness. Hypothermia, in which the body's core temperature drops below 35°C, can be caused by prolonged exposure to cold temperatures or certain medical conditions. Hyperthermia, in which the body's core temperature rises above its normal range, typically above 40°C, can be caused by heatstroke, extreme physical exertion, or certain medications.
Pulse Rate:
The normal resting heart rate range for an adult is between 60 to 100 beats per minute. A higher or lower heart rate may indicate a medical condition. Healthcare professionals use heart rate to assess cardiac function, diagnose heart conditions, and monitor the effectiveness of treatments.
Blood Pressure:
The normal blood pressure for an adult is typically around 120/80 mmHg. High blood pressure, or hypertension, is defined as consistently measuring higher than 130/80 mmHg, and can increase the risk of heart disease, stroke, and other health problems. Low blood pressure, or hypotension, is less common but can also be a serious medical condition, and is typically defined as a systolic pressure of less than 90 mmHg or a diastolic pressure of less than 60 mmHg.
Respiratory Rate:
The normal respiratory rate for an adult at rest is typically between 12 and 20 breaths per minute. A higher or lower respiratory rate than this range may indicate a medical condition. The quality of breath is also important in assessing a patient's respiratory function. Shallow, labored breathing or irregular breathing patterns can indicate respiratory distress and may require immediate medical attention.
Glasgow Coma Scale:
A GCS score of 15 is considered normal, indicating that the person is fully alert and oriented. The GCS is based on three categories: eye opening, verbal response, and motor response, and each category is assigned a score from 1-4 or 1-6. A higher score indicates a higher level of consciousness, while a lower score indicates a lower level of consciousness.
SPO2
Healthy SPO2 levels are between 95% and 100%, and SPO2 levels below 90% can indicate a lack of oxygen in the body. Supplemental oxygen may be necessary to raise the patient's SPO2 levels to a healthy range, but it is important to monitor the oxygen levels carefully and avoid over-oxygenation. Healthcare professionals use SPO2 measurements to guide treatment decisions and ensure that patients are receiving the appropriate level of oxygen.
Pupils:
The normal range for pupil size is between 2-4 millimeters in diameter for both pupils, and they should be equal in size. Pupils that are larger or smaller than this range, or are unequal in size (anisocoria), can be indicative of underlying medical conditions. Additionally, pupils should react briskly to changes in light, which is known as the pupillary light reflex. A sluggish or absent pupillary light reflex can be a sign of a neurological issue, such as a brain injury or nerve damage.
Skin:
Skin can vary in color and moisture depending on a person's age, sex, ethnicity, and overall health. In general, healthy skin should have a consistent color and texture across the body, without any unusual bumps, rashes, or lesions. The normal range of skin moisture varies from person to person, but it should generally feel soft and supple, without feeling excessively dry or oily.
Why First Responders Use Vital Signs?
Interpreting vital signs can help first responders make informed decisions about the best course of action for treating a patient. Monitoring changes in vital signs over time can also help to identify trends or progression of medical conditions, and inform treatment plans for better outcomes. First responders are trained to assess and respond to changes in vital signs quickly and effectively, which is essential in emergency situations.
At Delta Emergency Support Training we are happy to answer any questions you may have about vital signs as well as training sessions for individuals or classes. We offer in person, hybrid and online classes for Standard First Aid (SFA) Advanced First Aid (AFA) and Emergency Medical Responder (EMR) courses. For all inquiries please email info@deltaemergency.com .
Burn Management: Understanding Burns and How to Provide First Aid
Depending on the severity of the burn, it can be a painful and potentially life-threatening injury. Superficial burns only affect the outer layer of skin and typically result in redness, pain, and mild swelling. Partial-thickness burns affect both the outer and underlying layer of skin and can result in blisters, severe pain, and swelling. Full-thickness burns are the most severe type of burn, affecting all layers of skin and potentially even deeper tissue. Full-thickness burns can result in blackened or charred skin and can cause nerve damage, muscle and bone damage, and even death.
If you or someone else experiences a burn, providing first aid as soon as possible is crucial for promoting healing and preventing complications. The first step is to remove the source of the burn, such as a hot object or a chemical. Then, run cool (not cold) water over the burned area for at least 10-20 minutes. After that, cover the burn with a sterile, non-adhesive bandage or cloth. If the burn is severe, seek medical attention immediately.
A person's hand is shown with a burn on the skin. The person is using an antiseptic spray to clean and sanitize the burned area. The spray is shown being directed onto the burned area.
Burns are a common injury that can be caused by a variety of factors, including heat, chemicals, electricity, and radiation. Depending on the severity of the burn, it can be a painful and potentially life-threatening injury. It's important to understand the different types of burns and how to properly provide first aid and medical treatment to promote healing and prevent complications.
Types of Burns
There are three main types of burns, including superficial burns, partial-thickness burns, and full-thickness burns. Superficial burns only affect the outer layer of skin and typically result in redness, pain, and mild swelling. Partial-thickness burns affect both the outer and underlying layer of skin and can result in blisters, severe pain, and swelling. Full-thickness burns are the most severe type of burn, affecting all layers of skin and potentially even deeper tissue. Full-thickness burns can result in blackened or charred skin and can cause nerve damage, muscle and bone damage, and even death.
First Aid for Burns
If you or someone else experiences a burn, providing first aid as soon as possible is crucial for promoting healing and preventing complications. The first step is to remove the source of the burn, such as a hot object or a chemical. Then, run cool (not cold) water over the burned area for at least 10-20 minutes. After that, cover the burn with a sterile, non-adhesive bandage or cloth. If the burn is severe, seek medical attention immediately.
It's important to note that for chemical burns, it's important to flush the affected area with water for at least 20 minutes before removing any clothing or jewelry that may have come in contact with the chemical.
For electrical burns, it's important to turn off the power source or remove the person from the electrical source before administering first aid.
Medical Treatment for Burns
If a burn is severe or covers a large area of the body, medical treatment may be necessary. In addition to first aid, medical treatment for burns may include antibiotics to prevent infection, pain medication to manage discomfort, and intravenous fluids to replace lost fluids and electrolytes.
For partial-thickness and full-thickness burns, wound care may be necessary to promote healing. This can include removing dead tissue, applying topical creams or ointments, and using specialized dressings or wraps. In some cases, skin grafts may be necessary to cover the burn and promote healing.
For severe burns, such as those that cover a large portion of the body or involve the face, hospitalization may be necessary to provide more intensive care.
Preventing Burns
While it's not always possible to prevent burns, there are some steps you can take to reduce your risk. These include being careful when handling hot objects, wearing protective clothing when working with chemicals or other hazardous materials, and keeping children away from hot surfaces or objects.
Burns can be a painful and potentially dangerous injury, but with proper first aid and medical treatment, most burns can be effectively managed. It's important to understand the different types of burns, provide prompt first aid, and seek medical attention if necessary. By taking steps to prevent burns and following recommended burn management techniques, you can help protect your health and promote healing.
Assisting Elderly Who Have Fallen: A Comprehensive Guide to Providing Care and Support
Encountering an elderly or geriatric person who has fallen can be a difficult and distressing experience. Falls are a common problem among older adults and can lead to serious injuries, such as broken bones, head trauma, and bruises. It's important to approach the situation with care and sensitivity and take steps to provide appropriate assistance. Whether you're a family member, caregiver, or passerby, knowing what to do when you find an injured elderly person who has fallen can help to ensure their safety and well-being. In this blog post, we'll explore some general steps you can take to provide valuable assistance and help to ensure that the person receives the care and treatment they need.
Encountering an elderly or geriatric person who has fallen can be a difficult experience. It is important to approach the situation with care and sensitivity and take steps to provide appropriate assistance. Here are some general steps you can take to help:
two first aiders are providing assistance to an elderly person who has fallen. The first aider on the left is checking the person's pulse, while the other is evaluating their injuries. The person on the ground appears to be conscious but injured, and is lying on their side.
Evaluate the situation:
First, assess the situation to determine the extent of the person's injuries. If the person is conscious and can communicate, ask if they need help. If the person is unconscious or unresponsive, call emergency services immediately.
Provide first aid:
If the person has minor injuries that can be treated on-site, provide first aid as necessary. This might include cleaning and bandaging wounds, or helping them to sit or lie down in a comfortable position. If the person is bleeding heavily, try to apply pressure to the wound to stop the bleeding.
Call for help:
If the person's injuries are more serious or require medical attention, call emergency services immediately. Be sure to provide clear and accurate information about the person's location and the nature of their injuries.
Stay with the person:
While waiting for emergency services to arrive, it is important to stay with the person and provide comfort and reassurance. Let them know that help is on the way and that they are not alone.
Communicate clearly:
When speaking with the injured person, speak clearly and calmly. Avoid using complex language or medical jargon, and try to keep the person as relaxed as possible. If the person is unable to communicate, try to find out if they have any medical conditions or allergies that emergency services should be aware of.
Provide information:
If you are able to, provide emergency services with as much information as possible about the person's condition and any relevant medical history. This can help medical professionals provide more effective treatment.
Be respectful:
Remember that the injured person is likely to be feeling scared, vulnerable, and in pain. Treat them with respect and kindness, and try to keep them as calm and comfortable as possible until help arrives.
Encountering an elderly or geriatric person who has fallen can be a challenging experience, but by following these steps, you can provide valuable assistance and help to ensure that the person receives the care and treatment they need.Encountering an elderly or geriatric person who has fallen can be a difficult experience. It is important to approach the situation with care and sensitivity and take steps to provide appropriate assistance. Here are some general steps you can take to help:
Evaluate the situation:
First, assess the situation to determine the extent of the person's injuries. If the person is conscious and can communicate, ask if they need help. If the person is unconscious or unresponsive, call emergency services immediately.
Provide first aid:
If the person has minor injuries that can be treated on-site, provide first aid as necessary. This might include cleaning and bandaging wounds, or helping them to sit or lie down in a comfortable position. If the person is bleeding heavily, try to apply pressure to the wound to stop the bleeding.
Call for help:
If the person's injuries are more serious or require medical attention, call emergency services immediately. Be sure to provide clear and accurate information about the person's location and the nature of their injuries.
Stay with the person:
While waiting for emergency services to arrive, it is important to stay with the person and provide comfort and reassurance. Let them know that help is on the way and that they are not alone.
Communicate clearly:
When speaking with the injured person, speak clearly and calmly. Avoid using complex language or medical jargon, and try to keep the person as relaxed as possible. If the person is unable to communicate, try to find out if they have any medical conditions or allergies that emergency services should be aware of.
Provide information:
If you are able to, provide emergency services with as much information as possible about the person's condition and any relevant medical history. This can help medical professionals provide more effective treatment.
Be respectful:
Remember that the injured person is likely to be feeling scared, vulnerable, and in pain. Treat them with respect and kindness, and try to keep them as calm and comfortable as possible until help arrives.
Encountering an elderly or geriatric person who has fallen can be a challenging experience, but by following these steps, you can provide valuable assistance and help to ensure that the person receives the care and treatment they need.
At Delta Emergency Support Training we are happy to answer any questions you may have on geriatric emergencies as well as training sessions for individuals or classes. We offer in person, hybrid and online classes for Standard First Aid (SFA) Advanced First Aid (AFA) and Emergency Medical Responder (EMR) courses. For all inquiries please email info@deltaemergency.com .
Responding to Mass Casualty Incidents: A Guide for First Responders
Responding to Mass Casualty Incidents is a critical aspect of emergency preparedness and response. Whether it's a natural disaster, a terrorist attack, or an accident, the ability to quickly and effectively manage large numbers of injured victims can mean the difference between life and death. In such situations, emergency responders must work together to triage, treat, and transport the injured to medical facilities. They must also ensure that the scene is secure and that all necessary resources are available to address the needs of those affected.
Mass casualty incidents (MCIs) are situations where a large number of people are injured or killed at the same time. These incidents can be caused by natural disasters such as earthquakes, floods, or hurricanes, as well as by human-made events such as terrorist attacks or shootings. First responders play a crucial role in responding to these incidents and saving lives.
emergency responders in action, tending to multiple injured victims in a mass casualty incident. The responders are wearing protective gear and are working together to triage, treat, and transport the injured to medical facilities. The scene is chaotic, with debris and injured victims scattered around, highlighting the urgency and importance of effective mass casualty incident response.
Ensuring Safety: When responding to an MCI, the first priority for first responders is to ensure their own safety. They should always approach the scene with caution and be aware of potential hazards such as fires, explosions, or collapsing buildings. Once they have determined that it is safe to enter the area, they should quickly assess the situation and determine the number of casualties, the severity of injuries, and the resources needed to provide care.
Establishing Command: The first responders should then establish a command center to coordinate the response efforts. This center should be located in a safe area outside the immediate danger zone and should have clear communication channels with all response teams. The command center should also have access to emergency medical services (EMS) and transportation resources to move patients to hospitals or other care facilities.
Phases of Response: The response efforts should be organized into three main phases: triage, treatment, and transportation. During the triage phase, first responders should quickly assess each patient's condition and assign them to one of four categories: immediate (red), delayed (yellow), minimal (green), or expectant (black). Patients who are classified as immediate require immediate medical attention and should be transported to a hospital as soon as possible. Patients who are classified as delayed require medical attention but can wait for treatment. Patients who are classified as minimal require little or no medical attention, and patients who are classified as expectant are unlikely to survive even with treatment.
During the treatment phase, first responders should provide medical care to patients based on their triage category. Patients who are classified as immediate should receive the most urgent care, such as controlling bleeding, opening airways, or stabilizing fractures. Patients who are classified as delayed should receive medical attention as soon as possible, but their injuries are not life-threatening. Patients who are classified as minimal may receive basic first aid, such as bandages or pain relief. Patients who are classified as expectant should receive comfort care to minimize their suffering. During the treatment phase of a mass casualty incident, first responders should provide medical care to patients based on their triage category, which is determined during the triage phase. The triage categories are immediate (red), delayed (yellow), minimal (green), and expectant (black).
Patients who are classified as immediate require the most urgent care as their injuries are life-threatening and require immediate attention. First responders should prioritize stabilizing these patients by controlling any bleeding, opening their airways to ensure they can breathe properly, and stabilizing fractures or other injuries as quickly as possible. This may include the use of tourniquets, airway management devices, and splints.
Patients who are classified as delayed have injuries that are not immediately life-threatening but still require medical attention. First responders should provide medical care to these patients as soon as possible, but the urgency is not as high as it is for patients classified as immediate. For example, delayed patients may need pain relief, wound care, or treatment for broken bones.
Patients who are classified as minimal have injuries that are minor and may only require basic first aid, such as bandages or pain relief. These patients do not require immediate medical attention and can wait for treatment while more urgent cases are addressed.
Patients who are classified as expectant have injuries that are so severe that they are unlikely to survive even with medical treatment. First responders should provide comfort care to these patients to minimize their suffering, which may include pain relief, emotional support, and communication with family members or loved ones.
In summary, during the treatment phase, first responders should prioritize patients based on their triage category and provide the appropriate level of medical care to each patient. By following these guidelines, first responders can provide efficient and effective care to those in need during a mass casualty incident.
During the transportation phase, first responders should transport patients to hospitals or other care facilities based on their triage category. Patients who are classified as immediate should be transported first, followed by delayed patients. Minimal patients can be transported later or given transportation advice. Patients who are classified as expectant may not be transported, depending on the available resources and the patient's condition.
In conclusion, first responders play a critical role in responding to mass casualty incidents. They should always prioritize their own safety and quickly assess the situation to determine the resources needed to provide care. By following a structured approach that includes triage, treatment, and transportation, first responders can efficiently and effectively provide medical care to patients and save lives.
Emergency Transport How to Package a Patient Outdoors
Packaging a patient outdoors involves preparing the patient for transport while outside of a hospital or medical facility. This can be necessary if the patient is injured in a remote location, such as a hiking trail, or if the patient needs to be moved quickly due to a hazardous environment, such as a chemical spill. The process of packaging a patient outdoors requires careful planning and execution by trained emergency responders.
Once the situation has been assessed, the responders must stabilize the patient's injuries. This may involve applying pressure to a wound, immobilizing a broken bone, or providing oxygen to a patient who is having difficulty breathing. The goal is to ensure that the patient is as comfortable and stable as possible before transport.
Depending on the patient's injuries and the environment, there are several different methods for packaging a patient outdoors. Some of the most common methods include a vacuum mattress, a scoop stretcher, or a portable stretcher. The chosen method should be able to support the patient's weight and immobilize any injured limbs or body parts.
When it comes to emergency medical situations, time is of the essence. In some cases, patients need to be transported quickly, but the environment may not be suitable for immediate care. In these situations, packaging a patient outdoors can be a lifesaving measure.
Packaging a patient outdoors involves preparing the patient for transport while outside of a hospital or medical facility. This can be necessary if the patient is injured in a remote location, such as a hiking trail, or if the patient needs to be moved quickly due to a hazardous environment, such as a chemical spill.
Alberta emergency responder CREW stabilizing a patient's broken arm before packaging them for transport outdoors.
Here are the steps to properly package a patient outdoors for emergency transport:
1. Assess the Situation
Before any action is taken, the emergency responders must assess the situation. They must identify the extent of the patient's injuries and determine the best course of action for transport. They must also consider the surrounding environment and any hazards that may pose a threat to the patient or the responders.
Assessing the situation is the first and most important step in any emergency medical situation. When packaging a patient outdoors for emergency transport, it is crucial for emergency responders to assess the situation before taking any action.
Assessing the situation involves several critical steps, including identifying the extent of the patient's injuries and determining the best course of action for transport. The emergency responders must evaluate the patient's condition, taking note of any visible injuries, and gathering information about any underlying medical conditions or medications the patient may be taking.
Once the responders have assessed the patient's condition, they must also consider the surrounding environment. If the patient is injured in a remote location, responders must take into account the terrain, weather conditions, and the availability of resources. If the patient is in a hazardous environment, such as a chemical spill, responders must take steps to protect themselves and the patient.
Assessing the situation also involves considering any potential hazards that may pose a threat to the patient or the responders. This may include hazards such as falling debris, sharp objects, or dangerous wildlife. Responders must take steps to minimize these hazards and ensure the safety of everyone involved.
In some cases, the assessment may reveal that the patient requires additional medical resources or specialized care. In these situations, responders may need to call for additional support, such as a helicopter or specialized medical transport.
In conclusion, assessing the situation is a critical step in packaging a patient outdoors for emergency transport. By evaluating the patient's condition, considering the surrounding environment, and identifying potential hazards, responders can determine the best course of action for providing safe and effective care to the patient.
2. Stabilize the Patient
Once the situation has been assessed, the responders must stabilize the patient's injuries. This may involve applying pressure to a wound, immobilizing a broken bone, or providing oxygen to a patient who is having difficulty breathing. The goal is to ensure that the patient is as comfortable and stable as possible before transport.
Once the emergency responders have assessed the situation, the next critical step in packaging a patient outdoors for emergency transport is to stabilize the patient's injuries. Stabilization is essential to prevent any further damage to the patient's body during transport and to ensure the patient's safety and comfort.
The type of stabilization required will depend on the nature and severity of the patient's injuries. For instance, if the patient has a deep laceration, the responder may need to apply pressure to the wound to stop the bleeding. Similarly, if the patient has a broken bone, the responder may need to immobilize the affected limb to prevent further damage.
In some cases, the patient may require medical intervention to help stabilize their condition. For example, if the patient is experiencing difficulty breathing, the responder may need to provide oxygen to ensure the patient receives adequate oxygen supply.
The primary goal of stabilization is to ensure that the patient is as comfortable and stable as possible before transport. This will help to reduce the patient's pain and prevent any further complications during transportation. Proper stabilization can also help to prevent additional injuries that may occur during transport, such as further aggravation of a broken bone.
It is important to note that stabilization is not a substitute for medical treatment. Rather, it is a crucial step in preparing the patient for safe transport to a medical facility where they can receive further treatment.
In conclusion, stabilization is a critical step in packaging a patient outdoors for emergency transport. By identifying and stabilizing the patient's injuries, responders can ensure the patient's safety and comfort during transport, and help to prevent any further damage to the patient's body.
3. Choose the Packaging Method
Depending on the patient's injuries and the environment, there are several different methods for packaging a patient outdoors. Some of the most common methods include a vacuum mattress, a scoop stretcher, or a portable stretcher. The chosen method should be able to support the patient's weight and immobilize any injured limbs or body parts.
Choosing the appropriate packaging method is a crucial step in preparing a patient for safe transport outdoors in an emergency situation. The packaging method used will depend on the patient's injuries, the environment, and the available resources.
Some of the most commonly used packaging methods for outdoor transport include vacuum mattresses, scoop stretchers, and portable stretchers. Vacuum mattresses are ideal for patients with spinal injuries as they provide excellent support and immobilization. A scoop stretcher is typically used for patients with injuries to the lower body, while a portable stretcher is suitable for patients with injuries to the upper body.
Regardless of the packaging method chosen, it should be able to support the patient's weight and immobilize any injured limbs or body parts. The chosen method must also be able to withstand the rigors of outdoor transport, including uneven terrain and bumpy rides.
In addition to selecting the appropriate packaging method, it is essential to ensure that the patient is secured properly. Straps and restraints should be used to secure the patient in place, preventing any unnecessary movement during transport. The patient's head must also be immobilized to prevent any further injuries.
It is important to note that packaging a patient for outdoor transport requires specialized training and equipment. Only trained emergency responders should perform this procedure to ensure that the patient receives safe and effective care.
In conclusion, choosing the right packaging method is a critical step in preparing a patient for outdoor transport during an emergency. Emergency responders must carefully consider the patient's injuries and the environment to select the most appropriate method. By selecting the right method and securing the patient correctly, responders can provide safe and effective care during transport.
4. What gear should I use?
Vacuum Mattresses: These specialized mattresses are ideal for patients with spinal injuries or other injuries that require excellent support and immobilization. They work by creating a vacuum around the patient's body, conforming to their shape and providing optimal support during transport.
Scoop Stretchers: These stretchers are used for patients with injuries to the lower body, such as broken legs. They feature a hinged design that allows responders to gently scoop the patient onto the stretcher, minimizing any movement or further injury.
Portable Stretchers: These stretchers are designed for patients with injuries to the upper body, such as chest or head injuries. They are lightweight and compact, making them easy to carry to remote locations.
Straps and Restraints: To secure the patient to the chosen packaging equipment, responders may need straps and restraints. These should be tight enough to prevent any movement but not so tight that they cause discomfort or interfere with the patient's circulation.
Backboards: These rigid boards are used to immobilize patients with spinal injuries or suspected spinal injuries. They are often used in conjunction with other packaging equipment, such as scoop stretchers or vacuum mattresses.
It is important to note that emergency responders must be trained in the proper use of these packaging equipment to ensure that the patient receives safe and effective care during transport. The chosen method should be able to support the patient's weight and immobilize any injured limbs or body parts. The method used will depend on the patient's injuries, the environment, and the resources available.
5. Secure the Patient
Once the patient has been placed on the chosen packaging method, they must be secured in place. This may involve using straps or other restraints to prevent movement during transport. The patient's head must also be immobilized to prevent any further injuries.
Once the patient has been placed on the chosen packaging method, securing them in place is a critical step in preparing for outdoor transport. The primary goal of securing the patient is to prevent any unnecessary movement during transport that could cause further injuries.
The most common method of securing the patient is by using straps or restraints. The straps should be placed across the patient's chest, hips, and legs, ensuring that the patient is firmly secured to the packaging method. The straps should be tight enough to prevent any movement but not so tight that they cause discomfort or interfere with the patient's circulation.
In addition to using straps or restraints, the patient's head must be immobilized to prevent any further injuries. This is particularly important if the patient has suffered a head injury or has a suspected spinal injury. Immobilizing the head ensures that the neck and spine are protected during transport.
It is important to note that securing the patient is a delicate balance between ensuring their safety and not causing any further discomfort or harm. Emergency responders must be trained in how to properly secure a patient to avoid any potential complications during transport.
In addition to securing the patient, it is important to monitor their condition throughout the transport process. This includes regularly checking the patient's breathing, pulse, and level of consciousness. If any issues arise during transport, emergency responders must be prepared to take immediate action to address them.
In conclusion, securing the patient is a crucial step in preparing for outdoor transport during an emergency. Using straps or restraints to prevent movement, and immobilizing the patient's head are essential to ensure the patient's safety and prevent further injuries. Proper training and monitoring are also critical to provide safe and effective care during transport.
6. Move the Patient to Safety
With the patient securely packaged and stabilized, the responders can then move the patient to safety. Depending on the environment, this may involve carrying the patient to a nearby ambulance or using a specialized vehicle to transport the patient to a medical facility.
Once the patient has been stabilized, secured, and packaged for transport, the next critical step is to move the patient to safety. The method used to move the patient will depend on the patient's condition, the environment, and the resources available.
In some cases, the patient may be transported to a nearby ambulance or medical facility using a stretcher or other transport device. In other cases, specialized vehicles such as all-terrain vehicles, helicopters, or boats may be necessary to transport the patient.
When moving the patient, emergency responders must be careful to ensure that the patient remains stable and secure. They must also consider the environment and any potential hazards that may pose a threat to the patient or the responders. This may include navigating uneven terrain, avoiding obstacles, or taking steps to prevent further injuries during transport.
During transport, it is essential to monitor the patient's condition regularly. This includes checking their breathing, pulse, and level of consciousness. If any issues arise during transport, emergency responders must be prepared to take immediate action to address them.
Once the patient has been safely transported to a medical facility, the emergency responders must provide a detailed handover to the medical staff. This handover should include information about the patient's condition, any injuries or treatments provided during transport, and any other relevant information.
In conclusion, moving the patient to safety is a critical step in packaging a patient outdoors for emergency transport. Emergency responders must carefully consider the patient's condition, the environment, and any potential hazards to ensure safe and effective transport. Regular monitoring and a detailed handover to medical staff are also essential to ensure that the patient receives the appropriate medical care.
In conclusion, packaging a patient outdoors for emergency transport is a complex process that requires careful planning and execution. By following these steps and working as a team, emergency responders can provide the best possible care to the patient and ensure their safe transport to a medical facility.
At Delta Emergency Support Training we are happy to answer any questions you may have about Patient Packaging outdoors and Advanced First Aid. We provide training sessions for individuals or classes. We have options for in person, hybrid or online classes for Standard First Aid (SFA), Advanced First Aid (AFA), Emergency Medical Responder (EMR), and more courses. For all inquiries please email info@deltaemergency.com.
Unraveling the Mystery of the Heart's Electrical Dance: How Your Heart Beats to Its Own Rhythm!
Heart's Electrical Conduction - Key Concepts and Terminology. Delve into the intricacies of the heart's electrical conduction system with our comprehensive overview. Learn about the physiology, function, and regulation of the heart's electrical pathways. Gain a deeper understanding of this vital organ's complex conduction system with our informative blog.
Understanding the Intricacies of the Heart's Electrical Conduction System: A Comprehensive Overview
The human heart is a complex organ responsible for pumping blood throughout the body to sustain life. At the core of this remarkable organ lies a sophisticated electrical conduction system that coordinates the heartbeat and ensures its proper functioning. This paper aims to provide a comprehensive overview of the heart's electrical conduction system, including its anatomy, physiology, and the sequence of events that occur during each cardiac cycle.
Anatomy of the Heart's Electrical Conduction System: The heart's electrical conduction system comprises specialized cardiac cells that are distributed in various regions of the heart. These cells possess unique properties that enable them to generate, conduct, and regulate electrical signals, ultimately controlling the rhythm and rate of the heartbeat.
Sinoatrial Node (SA Node): The SA node is located in the upper right atrium near the opening of the superior vena cava. Often referred to as the "natural pacemaker" of the heart, the SA node initiates the electrical impulses that determine the heart's rhythm. It generates electrical signals that travel through the atria, causing them to contract and pump blood into the ventricles.
Atrioventricular Node (AV Node): The AV node is located at the bottom of the right atrium near the interatrial septum. It acts as a gatekeeper, delaying the electrical signals from the atria before passing them to the ventricles. This delay allows the atria to fully contract and empty their blood into the ventricles before the ventricles contract.
Bundle of His: The Bundle of His is a collection of specialized fibers that transmit the electrical signals from the AV node to the ventricles. It branches into the left and right bundle branches, which extend along the interventricular septum and eventually divide into smaller Purkinje fibers.
Purkinje Fibers: Purkinje fibers are specialized cardiac cells that distribute the electrical signals throughout the ventricles, causing them to contract and pump blood out of the heart.
Physiology of the Heart's Electrical Conduction System: The electrical activity in the heart is regulated by the flow of ions across the cell membranes of the cardiac cells, which results in changes in the cell's electrical charge. These changes in electrical charge create the electrical signals that propagate through the heart and coordinate the heartbeat.
Resting Membrane Potential: The resting membrane potential of cardiac cells is around -90 millivolts (mV), meaning that the inside of the cell is more negatively charged compared to the outside. This is due to the uneven distribution of ions across the cell membrane, with higher concentrations of potassium (K+) inside the cell and higher concentrations of sodium (Na+) and calcium (Ca2+) outside the cell.
Depolarization: The depolarization of cardiac cells is the process by which the cell's electrical charge becomes more positive, leading to the generation of an action potential. The depolarization of the SA node is initiated by the influx of calcium ions, which triggers the opening of voltage-gated sodium channels, allowing sodium ions to rush into the cell. This leads to a rapid depolarization of the cell membrane, resulting in the generation of an action potential.
Action Potential Propagation: Once the action potential is generated in the SA node, it spreads through the atria, causing them to contract. The action potential then reaches the AV node, where it is delayed for a brief period to allow the atria to fully contract and empty their blood into the ventricles. After the delay, the action potential is transmitted through the Bundle of His and the Purkinje fibers, which rapidly conduct the electrical signals to the ventricles. The depolarization of the ventricles leads to their contraction and the ejection of blood from the heart.
Repolarization: After depolarization, the cardiac cells need to repolarize to restore their resting membrane potential and prepare for the next electrical signal. Repolarization is achieved through the movement of potassium ions out of the cell, which results in the restoration of the negative charge inside the cell.
Sequence of Events during Cardiac Cycle:
The electrical conduction system of the heart plays a crucial role in coordinating the events of the cardiac cycle, which consists of two main phases: diastole and systole.
Diastole: During diastole, the heart is relaxed, and the chambers fill with blood. The electrical signals generated by the SA node initiate the diastole by causing the atria to contract and pump blood into the ventricles. The electrical signals then reach the AV node, where there is a slight delay before the signals are transmitted to the ventricles through the Bundle of His and Purkinje fibers. This delay allows for complete filling of the ventricles before their contraction.
Systole: During systole, the heart contracts, and blood is ejected from the ventricles into the arteries. The electrical signals from the Purkinje fibers cause the ventricles to contract and pump blood out of the heart. Once the electrical signals are completed, the heart returns to diastole, and the cycle restarts.
Regulation of the Heart's Electrical Conduction System: The heart's electrical conduction system is regulated by various factors to maintain the proper rhythm and rate of the heartbeat.
Autonomic Nervous System: The autonomic nervous system, consisting of the sympathetic and parasympathetic divisions, plays a significant role in regulating the heart's electrical conduction system. The sympathetic division increases the heart rate and conduction velocity, while the parasympathetic division decreases the heart rate and conduction velocity.
Hormones: Hormones such as adrenaline and noradrenaline released during times of stress or excitement can affect the heart's electrical conduction system, leading to an increase in heart rate and conduction velocity.
Electrolyte Balance: Proper electrolyte balance, particularly the levels of potassium, sodium, and calcium, is crucial for the normal functioning of the heart's electrical conduction system. Disturbances in electrolyte levels can disrupt the conduction of electrical signals, leading to arrhythmias.
The heart's electrical conduction system is a complex and intricate system that ensures the coordinated contraction and relaxation of the heart, leading to effective pumping of blood. The SA node acts as the natural pacemaker, generating electrical signals that initiate and regulate the heartbeat. The electrical signals are conducted through the AV node, Bundle of His, and Purkinje fibers, causing the atria and ventricles to contract in a synchronized manner. Proper regulation of the heart's electrical conduction system is essential for maintaining a healthy heart rhythm and preventing arrhythmias. Further research and understanding of this complex system may lead to advancements in diagnosing and treating various cardiac conditions related to electrical conduction abnormalities.
On the Frontline: Mastering Scene Assessment for AFA with Calgary & Edmonton Fire Departments
During an emergency, AFAs are trained to conduct thorough scene assessments to gather crucial information that informs the appropriate course of action. This includes assessing the safety of the scene, identifying hazards, evaluating the mechanism of injury or nature of illness, and determining the number of patients and their condition. By working closely with Calgary & Edmonton Fire Departments, we (EMS) can collaborate on scene management strategies, coordinate resources, and prioritize patient care based on the severity of injuries or illnesses.
Mastering AFA Scene Assessment with Calgary & Edmonton Fire Departments.
The safety of the AFA and the team is the top priority. Before entering the scene, the AFA should carefully assess for potential hazards, such as traffic, fire, hazardous materials, or violence. This may involve observing the scene from a safe distance to determine if it's safe to approach. If there are any immediate dangers, the AFA should take appropriate precautions, such as wearing PPE, using caution signs, and calling for assistance from, Police, EMS, Calgary Fire or Edmonton Fire departments, if needed.
as Advanced first aiders, Calgary FIRE & Edmonton Fire Departments always perform scene assessments during an emergency response.
Scene Size-Up: The AFA should assess the overall size and nature of the scene. This includes identifying the location, type of setting (e.g., residential area, workplace, public location), and any specific details that may impact the response, such as the presence of bystanders, vehicles, or potential sources of danger. This information helps the AFA get a general understanding of the situation and plan their approach accordingly, while coordinating with the Calgary or Edmonton fire department if necessary.
Mechanism of Injury or Nature of Illness: The AFA should observe and gather information about the mechanism of injury or nature of illness. This includes identifying how the injury or illness occurred, such as a motor vehicle accident, a fall, a medical emergency, or a traumatic injury. Understanding the mechanism of injury or nature of illness can help the AFA anticipate potential injuries or illnesses and determine the appropriate course of action for care, while keeping the Calgary or Edmonton fire department informed as needed.
Number of Patients: The AFA should assess the number of patients involved in the incident. This may include identifying if there are multiple patients or just one. This information helps the AFA determine the need for additional resources and prioritize care, while coordinating with the Calgary or Edmonton fire department to ensure adequate care for all patients.
Initial Impressions: The AFA should formulate an initial impression of the patients' condition(s) based on their observations from a distance. This includes looking for obvious signs of life-threatening conditions, such as unresponsiveness, difficulty breathing, severe bleeding, or obvious deformities. This initial impression can help the AFA prioritize care and initiate appropriate interventions, while keeping the Calgary or Edmonton fire department updated on the patients' status.
Additional Resources: The AFA should determine if additional resources are needed, such as additional EMS units, the Calgary or Edmonton fire department, or law enforcement. This may involve communicating with dispatch or calling for assistance from the Calgary or Edmonton fire department as necessary. The AFA should ensure that appropriate resources are enroute to the scene to provide timely and effective care.
Personal Protective Equipment (PPE): The AFA and the team should ensure that they are wearing appropriate PPE for the situation. This includes gloves, mask, goggles, and other protective gear as needed, to prevent exposure to potential hazards or communicable diseases. Wearing PPE is crucial to protect the AFA and the team from any potential risks during the response, while coordinating with the Calgary or Edmonton fire department for additional support if required.
Consideration of C-Spine: If there is a possibility of a spinal injury, the AFA should consider and maintain cervical spine precautions until further assessment can be performed. This may involve stabilizing the head and neck and avoiding any unnecessary movement that could worsen a potential spinal injury, while coordinating with the Calgary or Edmonton fire department for specialized assistance if needed.
Approach to Patients: The AFA should approach patients with care, assess their level of consciousness, and initiate appropriate care based on their assessment findings and protocols. This may include checking for responsiveness, assessing airway, breathing, circulation, and any obvious injuries. The AFA should provide care based on their training and protocols, while coordinating with the Calgary or Edmonton fire department for any additional support or specialized care that may be required.
Ongoing Assessment: The AFA should continuously reassess patients' conditions and monitor their vital signs, symptoms, and response to interventions. This includes checking for any changes in the patients' condition, identifying any new injuries or symptoms, and adjusting the care plan as needed. The AFA should communicate any changes or updates to the Calgary or Edmonton fire department and coordinate any necessary interventions or transport arrangements.
Documentation: The AFA should document their findings, assessments, interventions, and any communication with the Calgary or Edmonton fire department. This includes recording vital signs, patient information, and any other relevant details in the appropriate format or system. Accurate and thorough documentation is essential for continuity of care, communication with other healthcare providers, and potential legal purposes.
Handover to Higher Level of Care: If the patients require a higher level of care beyond the scope of the AFA's training or capabilities, the AFA should initiate handover to the Calgary or Edmonton fire department or other appropriate healthcare providers. This may involve providing a concise and accurate report of the patients' condition, care provided, and any pertinent details to ensure a smooth transition of care.
Scene Management: The AFA should actively manage the scene throughout the response, ensuring the safety of all individuals involved and coordinating with the Calgary or Edmonton fire department and other responding agencies as needed. This may include establishing a safe zone, controlling traffic, managing bystanders, and coordinating resources and logistics to ensure an efficient and effective response.
Follow-up: After the response, the AFA should debrief with the team, review the incident, and identify any areas for improvement. The AFA should also complete any necessary paperwork, reports, or documentation related to the incident, and follow any relevant protocols or procedures for reporting and follow-up. This may also include communicating with the Calgary or Edmonton fire department for any necessary follow-up or information sharing.
In conclusion, mastering scene assessment is a critical skill for Advanced First Aid (AFA) responders, and depending on your location, collaboration with Calgary Fire & Edmonton Fire Departments is crucial for efficient and effective emergency response. Through meticulous scene assessments, patient assessments, and accurate documentation, AFAs can work for fire departments and ensure scene safety and provide timely and appropriate medical care to those in need.
The partnership between AFAs and fire departments is vital in delivering excellence in emergency response on the frontline in Alberta. By continuously honing their skills and working together, AFAs and fire departments strive to provide the highest level of care to patients in emergency situations. It's important to remember that the roles and responsibilities of an AFA may vary depending on local regulations, protocols, and training. It's essential to always work within your scope of practice and seek appropriate guidance from your Fire department or other healthcare providers as needed.
At Delta Emergency Support Training we are happy to answer any questions you may have about Scene Assessments and Advanced First Aid. We provide training sessions for individuals or classes. We have options for in person, hybrid or online classes for Standard First Aid (SFA), Advanced First Aid (AFA), Emergency Medical Responder (EMR), and more courses. For all inquiries please email info@deltaemergency.com
What is an EMR?
The first step for an EMR is to assess the situation for hazards that can harm themselves, their partners, and their patients, and determine the nature of the emergency. They need to determine the level of medical attention needed and make quick decisions…
Behind the Scenes of an Emergency Medical Responder: Saving Lives with Speed and Skill
An Emergency Medical Responder (EMR) is a healthcare professional who is trained to provide immediate medical care in emergency situations. EMRs are often the first healthcare providers to arrive on the scene of an emergency, and they work closely with other healthcare professionals to ensure that patients receive the appropriate care and treatment. EMRs are trained to provide basic life support measures, including administering CPR, controlling bleeding, treating shock, managing spinal injuries, and stabilizing fractures. They are also trained to manage patients with a variety of medical emergencies, including cardiac arrest, respiratory distress, and trauma. Here are some of the typical job functions of an EMR:
1. Assess the situation:
The first step for an EMR is to assess the situation for hazards that can harm themselves, their partners, and their patients, and determine the nature of the emergency. They need to determine the level of medical attention needed and make quick decisions based on their assessment.
2. Stabilize Patients:
EMRs are trained to stabilize patients by maintaining their airways and providing necessary interventions such as assisted ventilations, medical oxygen, life-threatening bleeding, and medication.
2. Administer First Aid:
EMRs are trained to provide basic-intermediate-advanced first aid such as CPR, wound management, and immobilization of injured patients.
4. Communicate with the medical team:
EMRs communicate vital information to the medical team, such as the patient's vital signs, symptoms, and any other relevant medical history.
5. Provide Emotional Support:
EMRs provide emotional support to patients and their families during times of crisis. They should be compassionate and empathetic, helping to ease the stress and anxiety that often come with medical emergencies.
6. Document the incident:
EMRs must document the incident, including vital signs, patient history, and any medical interventions administered.
7. Transport Patients:
EMRs are responsible for transporting patients to medical facilities safely. Overall, the role of an EMR is crucial in emergency medical situations, and they must be well-trained, quick-thinking, and compassionate individuals. EMRs work in a variety of settings, including ambulance services, fire departments, and hospitals. They play a critical role in the healthcare system by providing immediate medical care to patients in emergency situations, and their actions can often make the difference between life and death.
The road to EMR certification can be confusing. The EMR program is different in provinces like BC, Alberta, Saskatchewan, and Manitoba. The Canadian Red Cross EMR, AFA, or FR curriculum is identical across Canada but provincial standards and must be taught in respective provinces. At Delta Emergency, we understand what certifications you need for your future career, how and where to obtain them, and what type of work will be available to you when you’re fully certified. Reach out with questions!
BVM
Maintain an Airway, use HTCL or MJT, use Suction, insert an OPA or NPA, begin Ventilations and apply Oxygen. BLS, FR, AFA, and EMR
This is a basic and generalized overview of Emergency Medical Responders across North America. When in doubt, follow your local protocols! Contact us if you have any specific questions about the EMR scope of practice and career path in Alberta. We are industry experts and have been working full time in EMS for years.
At Delta Emergency Support Training we are happy to answer any questions you may have about becoming an EMR. We provide training sessions for individuals or classes. We have options for in person, hybrid or online classes for Standard First Aid (SFA) Advanced First Aid (AFA) and Emergency Medical Responder (EMR) courses. For all inquiries please email info@deltaemergency.com
SMR - Spinal Motion Restriction | Professional Responder Skill Series
While SMR is generally considered a safe and effective method for preventing spinal cord injury, there are certain risks and considerations that must be taken into account, such as the potential…
"Spinal Motion Restriction: Techniques and Considerations for Prehospital Care Providers"
Spinal motion restriction (SMR) is a technique used to limit movement of the spinal cord and surrounding tissues during transport to a medical facility for further evaluation and treatment. SMR is typically performed by prehospital care providers, such as paramedics or emergency medical technicians, who are trained in the technique and can quickly assess and stabilize a patient's condition.
SMR involves the use of various devices and techniques to immobilize the spine, including cervical collars, backboards, and straps. While SMR is generally considered a safe and effective method for preventing spinal cord injury, there are certain risks and considerations that must be taken into account, such as the potential for pressure ulcers, respiratory compromise, and the need for prompt removal of SMR devices once the patient reaches a medical facility. Prehospital care providers must also be aware of the latest guidelines and protocols for SMR, as these may vary depending on the patient's condition and the severity of their injuries.
In addition to trauma patients, individuals with certain medical conditions may also require SMR. For example, individuals with spinal fractures, spinal tumors, or spinal infections may require SMR to prevent further damage to the spine and surrounding tissues.
It is important to note that SMR should only be performed by trained professionals and should be used judiciously, as excessive immobilization can lead to complications such as pressure ulcers, respiratory problems, and muscle atrophy.
Ultimately, the decision to use SMR should be made on a case-by-case basis, taking into account the patient's specific needs and the risks and benefits of this technique. In some cases, SMR may be necessary for the safety of the patient, while in other cases, alternative techniques may be more appropriate.
AHS First Responder C-Spine Protocol
This section contains a large amount of information about how we determine applying SMR to a patient. As a firefighter or first responder in Alberta, this is the protocol you will also follow. If you examine both the Canadian C-Spine rule and the AHS C-Spine Protocol, you will find they are very similar.
Background
The C-Spine Assessment Protocol is to be applied to blunt trauma patients where there is a potential for a cervical spine injury and/or the potential for pre-hospital C-spine clearance where the practitioner needs to assess the requirement for spinal motion restriction (SMR). It is imperative that the practitioner primarily assesses the patient and not the scene or mechanism to determine the need for SMR. To facilitate this, the Canadian C-Spine Rule has been incorporated into the protocol to aid practitioners’ decision-making.
The Canadian C-Spine Rule applies to alert (GCS of 15), cooperative, and stable adult blunt trauma patients where there is a potential for C-spine injury with neck pain and/or trauma markings above the level of the clavicles.
C-collar application and SMR are contraindicated in all cases of isolated penetrating trauma. C-collar application and SMR are NEVER indicated in any isolated penetrating trauma. There is documented increased mortality due to the delay to definitive care with surgical interventions as a result of increased on scene time while applying C-collar and SMR. Of note, the long board can still be used to facilitate the extrication of the patient.
Patient Safety Considerations
SMR and C-collar application are contraindicated in cases of isolated penetrating trauma. For those patients greater than 65 years of age, take into account biological age versus chronological age. An alert, cooperative and stable patient with no neurological symptoms and no neck pain can be transported without a C-collar. The long board is not necessary for SMR
Etiology
This algorithm is designed to help the practitioner make an informed determination of the need for spinal motion restriction in the field. It is for alert (GCS of 15) and stable trauma patients where cervical spine injury is a concern.
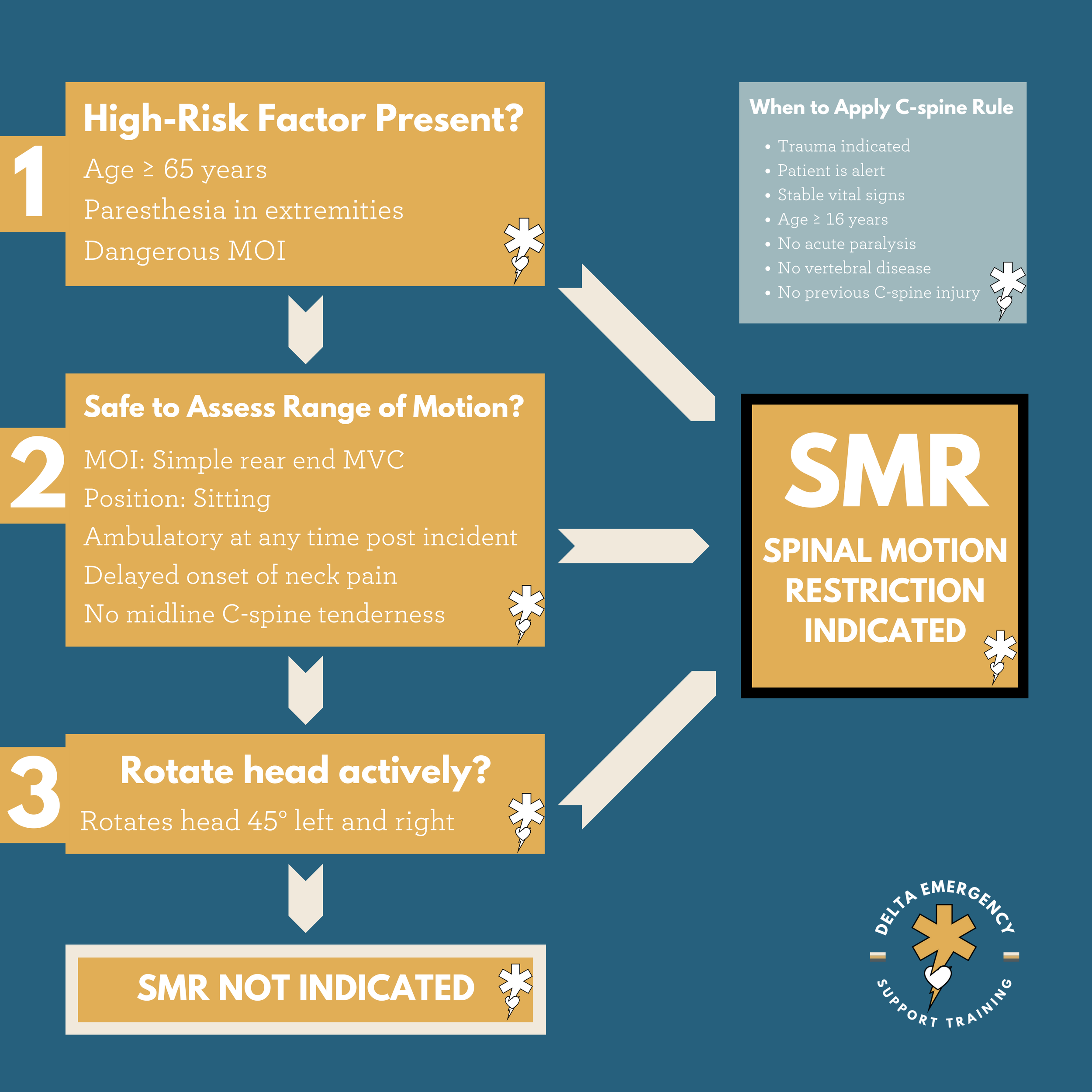
Perform spinal motion restriction (SMR) if any of the following are present:
High-risk factors
Fall from 1 m / 5 stairs or greater
Axial load to head (e.g. diving injuries)
MVC (Speed greater than 100 km/h, rollover, ejection)
Motorized recreational vehicles
Bicycle collision with object
Medical risk factors (for example, arthritis, prolonged steroid use, degenerative bone disease, history of cervical surgery)
MVC with death of other occupant in the same vehicle
Collisions involving ATVs, motorbikes, and snowmobiles
Pedestrian/cyclist struck by motor vehicle at greater than 15 km/h
Altered LOC
Glasgow Coma Scale 14 or less
Disorientation to person, place, time, and/or event
Inability to remember 3 objects after 5 minutes
Delayed or inappropriate response to external stimuli
Paresthesia – including any abnormal motor or sensory neurological finding (e.g. numbness, tingling, weakness)
Unequal handgrip strength
Inability to raise arm(s) against gravity
Inability to move toes
Inability to perform plantar flexion and dorsiflexion of the feet
Sensory deficits such as weakness or numbness or radicular (electric or shooting) pain
Tenderness/deformity of spine
Almost all spinal injuries are associated with either pain or tenderness localized to the spine
Pain felt deeply in the neck should be considered spine pain
Alcohol/drugs affecting judgement
Communication difficulties (e.g. language barrier)
Distracting painful injury:
Long bone fracture
Abdominal or thoracic injury causing distress
Large laceration, degloving, or crush injury
Large burns
Any other injury-producing acute functional impairment
Degenerative bone disorder, ankylosing spondylitis, Down’s syndrome – assure the neutral position corresponds to the underlying medical condition
Suspicion of spinal injury on the part of the practitioner
If any of the following low-risk factors for spinal injury are present, evaluate patient for need for spinal motion restriction:
Ambulatory at any time
Absence of pain during midline palpation
Delayed (not immediate) onset of neck pain
Simple rear-end MVC, excluding:
Pushed into oncoming traffic
Hit by bus / large truck
Rollover
Hit by high-speed vehicle (100 km/hr or greater)
On evaluation, if unable to voluntarily rotate the neck 45° left and right, regardless of pain, use SMR.
Range of Motion Examination
Ask the patient to voluntarily rotate their neck 45° to the left and right regardless of pain
If the patient can rotate their neck, spinal motion restriction is not indicated\
Nerve Root | Movements
C5 | Shoulder adbuction, elbow flexion
C6 | Elbow flexion (semipronated)
C7 | Finger extension, elbow extension
C8 | Finger flexors
T1 | Small muscles of the hand
L1, L2 | Hip flexion
L3, L4 | Knee extension
L5 | Extension of great toe
S1 | Hip extension, knee flexion, plantar flexion
Don’t forget sensory — light touch/pain
Spinal motion restriction (SMR)
SMR is required in all patients with potential spinal injuries, with the exceptions as above (i.e. penetrating trauma)
Where possible, SMR should be maintained with a properly fitted C-collar and/or blanket-rolls (or a comparable commercial device) secured to the stretcher with tape when appropriate. If a c-collar would pull the patient out of neutral alignment then it should not be applied
Supine positioning is the preferred position for patients requiring SMR. However, if these patients cannot be transported supine, they should be maintained in a reasonable position of comfort with neutral alignment of the spine relative to the patient’s underlying medical condition or their current presentation
SMR should not take priority over management of life-threatening co-morbidities such as airway management or hemorrhage control
Long boards can be used for extrication or as a means of moving an immobile patient to the stretcher but is not required to achieve SMR and is contraindicated in patients who have a long transport and/or wait times (greater than 30 minutes)
EMS practitioners may remove the patient from the long board and place them supine with a C-collar and head rolls/head blocks, onto an EMS stretcher (secured with stretcher seatbelts), as soon as deemed safe and practical to do so
In cases in which SMR is indicated as per protocol, patients with life-threatening respiratory compromise exacerbated by the supine position (i.e. head, facial/neck trauma, severe respiratory disease, body habitus), may be transported on the stretcher in semi-Fowlers or high Fowlers (maintaining SMR with a C-collar/head blocks and secured with stretcher seatbelts
Patients with C-collars in place should not be transferred via wheelchair or walking
With regard to the pillow/padding of SMR patients, the priority is maintaining neutral alignment as near as possible. Continue with light padding or small pillows which do not alter the normal cervical alignment of patients as long as the SMR techniques still ensures appropriate control, immobilization and stabilization of the C-spine
Once again: C-collar application and SMR are contraindicated in all cases of isolated penetrating trauma. C-collar application and SMR are NEVER indicated in any isolated penetrating trauma. There is documented increased mortality due to the delay to definitive care with surgical interventions as a result of increased on scene time while applying C-collar and SMR. Of note, the long board can still be used to facilitate the extrication of the patient
The information above is opinion based and taken from different research articles, First Response training protocols, AHS EMS, and textbooks. There are no specifics given regarding an assessment or treatment modality, as SMR protocols change between different Fire/EMS systems. Follow YOUR local protocols.
At Delta Emergency Support Training we are happy to answer any questions you may have about spinal motion restriction. We provide training sessions for individuals or classes. We have options for in person, hybrid or online classes for Babysitters, Standard First Aid (SFA) Advanced First Aid (AFA) and Emergency Medical Responder (EMR)courses. For all inquiries please email info@deltaemergency.com
Calgary and Edmonton Fire Applications Opening in 2022 and 2023!
So you meet the minimum requirements to apply for Calgary and Edmonton Fire. What certifications do you need before you’re given a job offer? Canadian Red Cross Advanced First Aid is one of the certification requirements, and at Delta Emergency, we fully certify you to Alberta Fire Department standards.
Are you looking to change careers and apply with Calgary Fire or Edmonton Fire? Calgary Fire opened their recruitment on November 1, 2022 and it closes on November 30, 2022! Edmonton Fire will be opening their recruitment process from January 1-31, 2023.
If you haven’t taken Advanced First Aid (AFA) within the last 3 years, you will need to certify in an AFA course prior to a conditional job offer from either fire department. Here at Delta Emergency Support Training, we certify you as a Canadian Red Cross Advanced First Aider with Basic Life Support (BLS CPR) in one course.
Our AFA course is a hybrid version, perfect for individuals with full-time jobs, families, or busy schedules. There are 40 hours of online virtual sessions/online work to complete, and 40 hours of in-person skill days.
We typically run an AFA Cohort over the course of 4-6 weeks, and you attend 2 Friday nights and 2 weekends with our full-time active duty Advanced Care Paramedic instructors. We have real experience, real equipment, and exceptional student feedback.
Be one of our next students and become a Professional Responder.
Calgary Fire: Do you meet the minimum requirements to apply?
Be 18 years of age or older
Be a Canadian citizen or permanent resident
Have a high school diploma or equivalency
Have a valid Class 5 driver's license or provincial/territorial equivalent without a Graduated Driver’s License (GDL) status and with less than 7 demerit points
Have been granted a pardon or record suspension for any criminal convictions.
Meet all immunization requirements
Have a maximum of one illegal soft drug use in the past year and a maximum of three illegal soft drug uses in the past 3 years. Candidates must have had zero hard drug use in the past three years.
Edmonton Fire: Do you meet the minimum requirements to apply?
Applicant must be at least 18 years of age
Applicant embraces and actively promotes the behaviour and values of an inclusive, diverse and respectful work environment.
It is a requirement to obtain and maintain a City Driver's permit.
An overall satisfactory driver's record is required upon hire.
Hire is dependent upon a satisfactory Vulnerable Sector Police Information Check.
Good physical fitness is required and is evaluated at the fitness test stage.
Ability to understand and communicate clearly and concisely in English under stressful conditions.
Delta Emergency Hybrid Red Cross Advanced First Aid
We started teaching this new version of Hybrid Advanced First Aid in June 2021. Every student has rated our program with 5 stars and they all recommend it to their peers. 60 hours of at home learning and 24 hours in-class over 1 Friday night, Saturday and Sunday. Certify as an Advanced First Aider through online content such as videos, skill sheets, quizzes, written group discussions, 1:1 video instructor video sessions, weekly workbooks - more than multiple choice questions, games and repeatable tests to test your comprehension. Real instructors with real emergency experience. Skill sessions that deliver quality scenarios. Group scenarios to develop real world teamwork.
Delta Emergency Canadian Red Cross Hybrid Advanced First Aid
We started teaching this new version of Hybrid Advanced First Aid in June 2021. Every student has rated our program with 5 stars and they all recommend it to their peers. 60 hours of at home learning and 24 hours in-class over 1 Friday night, Saturday and Sunday. Certify as an Advanced First Aider through online content such as videos, skill sheets, quizzes, written group discussions, 1:1 video instructor video sessions, weekly workbooks - more than multiple choice questions, games and repeatable tests to test your comprehension. Real instructors with real emergency experience. Skill sessions that deliver quality scenarios. Group scenarios to develop real world teamwork. We’re a smaller business of like-minded emergency professionals and we’re not listed on Google, yet.
Traditional Canadian Red Cross Advanced First Aid
What does 80 hours in the classroom look like? Sitting in a classroom for 10 days straight. Taking vacation days or quitting your job. Past Red Cross Advanced First Aid students with other providers have let us know they feel they're being kept in class just to hit that 80 hour requirement and feel the in-person course is too long. The other downside is that the first 5-6 hours of each day are focused on the didactic training and PowerPoint, then you practice 1 or 2 skills at the end of the day. Traditional classroom works for some people. We are here to accommodate the people that need a true Hybrid Learning Format with 1 weekend of in-person skills.
Friday Night Session
Here's how Friday looks:
Arrive at weekend training facility. Give an overview of classroom setup. Student and instructor introductions.
Review quizzes, exams, answer questions from online course. Jeopardy style game for course content review.
Review any skills sheets that were unclear. Speak about skill indications + contraindications.
Practice taking vital signs - pulse, blood pressure, respiratory rate, lung sounds, SpO2, etc.
Discuss Week 3 verbal scenario, verbal scenario performed as a group.
Saturday + Sunday Session
Here’s a brief overview of Saturday:
All other AFA skills are demonstrated by the instructor and then performed by each student.
Individual and group scenarios are given throughout the day.
Group skills such as spinal motion restriction will require the student the participate in the skill at least 4 times.
Once to run the skill, and other times being part of a team member running the skill.
Every skill learned is applied to scenarios on Sunday.
Here’s a brief overview of Sunday:
Scenario day. Every scenario is graded. You need 1 successful scenario where you are the primary attendant to pass the course.
Scenarios will build in complexity. Basic ones at first to solidify the Scene/Primary assessments. Memorization of Assessment Acronyms is key.
Scenarios then progress in patient severity, where all team members work together to apply skills/equipment.
You will use more than 1 piece of equipment and skill as scenarios progress. The goal is to use the equipment realistically every single time.
You will be asked key knowledge points about each piece of equipment when you utilize them.
Key points were taught through the online course, textbook reading, the workbooks, quizzes, skill sheets, and Friday/Saturday.
Private Video Session with an Instructor
Does every student recommend the video session? Yep.
Does any other AFA provider offer 1:1 video sessions with their students? Nope, just Delta Emergency.
There are virtual time-slots for everyone to have a 1+ hour session with an instructor prior to the in-person course. It is capped at 1 student per session. It is not required, but recommended. Sometimes they go to 90+ minutes, but we've had great feedback from students that have signed up for the video session. In the session, we can review your course progress, review mid-terms/quizzes, and clarify any questions.
Then, we review how in-person scenarios are structured and we give you a basic verbal scenario during the hour. It will help you understand the format of what we are looking for during your scenarios. Availability will be on weeknights after 18:00. The online scheduler for this will be available within the online course. There will be as many spots open as there are students in each cohort.
Weekly Written Scenarios
At the start of Week 1 and Week 2 we release a scenario writeup that describes an emergency call and some basic scene and patient information.
All students will read the scenario and reply to the scenario. Students think about the first steps they would take and their initial treatments. They type what they would do from Scene Assessment -> Treatments.
Students write their own reply, can format is however they like, and do not reply with "I'd do what she did, and add..."
Instructors will read each students answer but not reply until everyone has completed the assignment. Students have 1 week to writeup a reply to each week.
The goal is to see what you prioritize and what you visualize as potential treatment/patient pathways. We give feedback on what you wrote. It doesn't matter if you forgot C-Spine, or didn't think about shock, etc. It is used as a learning tool and is a great way to see the priorities you fellow classmates think about.
We release a formal writeup and answer to the scenario 10 days after one is posted. It contains all the things a student could consider with that particular emergency. There are actually some key points to take away as you work in the real world and encounter similar patients.
The Future
We want to be the first Red Cross provider that stays connected to their past students. Delta Emergency Professional Responder Community Forum. The goal is to make it a space for students to connect, make a concise list of emergency medical pathways for programs/colleges/provinces, share volunteering opportunities, career postings, first responder discounts, real-call talk, scenarios, etc. It will be a place that only past students can access, so there won't be any internet trolls - unless you are one. We just wanted to make a dedicated training spot for you to come and reflect on different emergency calls.
Want to use a BVM again? SMR a patient to a backboard? The Delta Community Forum will also keep you informed of joining in-person skill days. There will be a small fee to cover some basic costs, but it will allow you to come for the full weekend, or just 1 day of scenarios on Sunday. After class registration closes for a cohort we will contact past students through our LMS and invite them to come back for some risk-free, stress-free training.
The Delta Community Forum will also be a perfect way to introduce yourself to other students, network, and possibly exchange information about training, volunteering, or job opportunities. It's up to you. A network of Professional Responders lifting one another up. What could be better?
Update Nov 19, 2021: We are currently modifying our format and more details will be released in January 2022.